Rosacea is a very common and troublesome condition that affects many people. It has been estimated to affects at least 6% of the population and up to 10% of people with fair complexions. Rosacea is often underdiagnosed in people with skin of colour. Women are affected 2-3 more frequently than men, but men tend to suffer more severely from the disease. Rhinophyma which is the bulbous projection of the nose occurs almost exclusively in men.
The most common and annoying features are the flushing, persistent redness, papules, pustules and the intolerable burning sensation. Patients with rosacea often experience distress, anxiety, guilt, embarrassment, low self-esteem, depression, and a poor body image.
A negative impact on relationships, poor sleep and an impaired concentration at work appears to be associated with the disease.
Fear of unpredictable flushing of the face can be stressful, embarrassing and debilitating, trapping sufferers in a cycle where the stress from flushing flares just makes the flushing worse, further increasing fear of social rejection.
Rosacea suffers not only have to manage their own negative self-image but also negative perceptions and reactions from others.
What are the features of rosacea?
Major features include flushing, papules and pustules and telangiectasia. Eye symptoms include dilated vessels along the eyelid margin as well as other ocular features.
Minor features include burning sensation, stinging sensation swelling, dryness and a honey crust accumulating at the base of the eyelashes. Irregularities of the eyelid margin including rapid tear break-up time are other features of ocular rosacea.
Management of rosacea
Rosacea is a chronic condition with exacerbating factors. The goal is initial improvement followed by long term maintenance of the condition. Education of this condition is important in the management.
Diet
Triggers of rosacea include ingestion of hot foods and drinks as well as alcohol mainly red wine. Other triggers also include exposure to heat, sunlight and irritating skin care products have also been implicated. Capsaicin is found in spicy foods and includes sauces, cayenne and red peppers. Cinnamaldehyde is found in a range of foods such as tomatoes, chocolate and citrus foods which can lead to aggravation of rosacea. Niacin- containing foods such as turkey, peanut, tuna, liver and chicken have also been implicated to cause flushing. Dairy products such as yoghurts, sour cream and cheese but not cottage cheese as well as chocolate, vanilla, soya sauce and yeast extracts but not bread, vinegar, eggplant avocado, spinach, beans, bananas, Red plums, raisins and figs have also been implicated to exacerbate symptoms of rosacea in some patients.
Can any dietary manipulation help the rosacea?
Zinc and Omega 3 fatty acids have been shown in small studies to the anti-inflammatory and therefore may improve rosacea. One trial showed improvement after dietary supplementation of zinc sulphate 100 mg 3 times a day. Omega-3 fatty acids are known to inhibit proinflammatory pathways. Significant improvement was seen in one study in patients with rosacea who ingested 325 mg of omega-3 fatty acids as well as a reduced dose of 175 mg daily for 3 months.
Treatment of rosacea
We recommend baseline photographs of the face including frontal, oblique left and light views. This will allow the patient to document the improvement with treatment.
Topical therapy
Pustular papular rosacea is usually managed with topical therapy alone. This may include metronidazole gel or cream. It is recommend you apply the gel cream twice a day for up to 3 to 4 months and is safe in pregnancy.
Azelaic acid in 15% concentration in gel or foam or 20% in cream has been shown to be effective in multiple trials for the treatment of papular pustular rosacea. Azelaic acid can be more irritating and then metronidazole. In Australia 15% azelaic acid gel was shown to be similar in efficacy to 1% metronidazole gel but is superior to 0.75% metronidazole gel. In Australia 15% azelaic acid gel and 20% azelaic acid lotion are approved. They were both safe to use during pregnancy.
Ivermectin cream has been used in papulopustular rosacea. It is also effective in treating Demadex infection of the skin. Mild stinging and burning sensation can occur on application. It is a category C in pregnancy. Ivermectin cream should be used for an extended length of time up to 24 weeks for maximum improvement.
Brimonidine tartrate is 8 potent vasoconstrictor and is effective in reducing facial redness in rosacea. It is available 0.33% gel and has applied once daily. A reduction in redness is seen within 30 minutes of applying the gel.
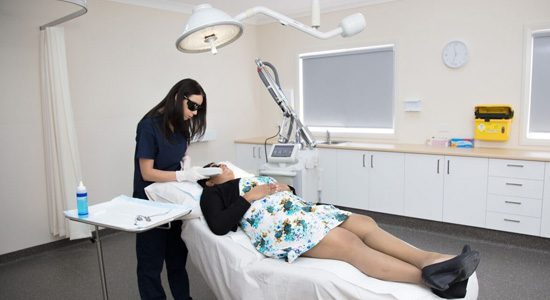
IPL
Intense Pulse Light therapy has been shown to be effective in young patients with more severe rosacea and with significant redness and dilated blood vessels (erythematous and telangiectasia)
Long pulsed NdYAG laser 1064nm
At high fluence 40-50mJoules and 50 msec NdYAG laser can reach depths of 4-6mm where there are deep telangiectatic blood vessels. There is also dermal rejuvenation and reduction of wrinkles by dermal collagen remodelling which is induced by non-selective bulk heating of the dermis.
Both devices are available at our dermatology practice.
Pregnancy and rosacea
For mild-to-moderate rosacea azelaic acid has been shown to be safe during pregnancy. In more severe cases of rosacea erythromycin orally can be used safely. Erythromycin is generally considered safe during any stage of pregnancy when administered for a few weeks.
Oral treatment during first trimester is best avoided. Oral treatment should be limited to 4 to 6 weeks of therapy.
LED light is considered safe during pregnancy.
Kleresca gel and LED light activation is also considered safe for the management of rosacea in pregnancy.
Basic skin care regimen for patients with rosacea
1. Use a gentle cleanser pH 5.5.
2. Avoid products that contain fragrance, colours and essential oils as they can increase the likelihood of skin irritation.
3. Wear sunscreen SPF 50. Sun exposure is known to trigger or exacerbate rosacea. A facial moisturiser containing sunscreen SPF 50 would be adequate.
What are the causes of rosacea?
- Genetics
There is a higher incidence in people of Northern-European descent particularly the Celtic population. One third of patients with rosacea have a family history of this condition.
- Environmental factors
Increased environmental temperature and dietary factors can exacerbate rosacea. Hot spicy food, hot beverages, UV exposure, exercise and emotional stress can trigger the condition.
Alcohol can act as a trigger for rosacea by affecting the gut microbiome, activate inflammasomes TLR-2 and TRPV1, and therefore propagate the inflammatory cascade.
- Biological factors
This include demodex mites, cutaneous or GI bacteria, an impaired gut microbiota such as small intestinal bowel overgrowth syndrome and stomach infection due to Helicobacter pylori.
- Demodex
Demodex folliculorum is a commensal mite that lives in or near the pilosebaceous units in human skin. This mite is found in higher density in skin affected by rosacea than in controlled skin.
- Bacteria
Staphylococcus epidermidis has been shown to be increased in skin affected with rosacea. Whether this organism plays a role in the cause of rosacea is yet to be determined.
- Gastrointestinal microorganisms
The intestinal microbial population may have an effect on human skin. The mechanism remains incompletely understood. There is evidence in the medical literature that certain foods such as fermented foods, kefir and kimchi, as well as probiotics that promote microbiome diversity have accelerated clearance of both helical factor pylori and improved rosacea. It is unclear whether there is a pathogenic link between Helicobacter pylori infection and rosacea.
- Immune responses
Skin barrier dysfunction.
There is increased transepidermal water loss and a rise in facial pH in the skin affected by rosacea.
There is an up regulation of various inflammatory mediators such as the release a pro-inflammatory cytokines in the skin of patients with rosacea. This leads to angiogenesis involving blood vessel formation.
Oral therapy
Doxycycline 50 to 100 mg daily is effective as an initial treatment of rosacea. Atypical course would be over a period of 6 to 12 weeks alone or in combination with topical therapies. Potential adverse side effects include dose-related photosensitivity and oesophagitis. To minimise photosensitivity a broad-spectrum sunscreen SPF 50 and a broad brim hat are recommended.
Minomycin 50 to 100 mg has also been shown to be effective. A prescribed course of 4 to 12 weeks have been recommended.
Tetracyclines in doses of 250 to 500 mg daily have also been used for a period of 4 to 12 weeks. Tetracyclines classified as category D in pregnancy.
Alternatives to Tetracyclines include macrolides such as erythromycin and less commonly azithromycin, clarithromycin and clindamycin have also been prescribed in rosacea.
Erythromycin is commonly prescribed for pregnant women beyond the first trimester and can be used in breastfeeding. It is a category A drug in pregnancy.
Isotretinoin in low doses of 5 mg daily have been shown to be helpful in the reduction of papules and pustules. A minimum duration of 3 to 4 months is often required.
Prognosis
Rosacea is a chronic condition with exacerbating factors. The aim of treatment is to effectively manage this condition and minimise the progression of symptoms. This condition can wax and wane. The aim is for the patient to take control their condition by educating the patient by providing good quality information on this condition as well as a clear management plan
Medications can take time to become effective and improvement can be slow. Misconceptions such as rosacea is due to poor hygiene or excessive drinking need to be put at rest.
Educating friends, family and colleagues about their condition can help to minimise distress.
