Newer treatments that are at the cutting edge for treating acne using photobiomodulation are now available at our practice. This new treatment uses visible light to trigger biological reactions in the skin through a photochemical pathway. The light source used include light emitting diode LED therapy incorporating a blue and red light. Another treatment that we have recently introduced is using a chromophore containing gel applied to the skin which is activated by another LED lamp that emits a fluorescent light. Both treatments are available at our practice.
Photodynamic therapy using a photosensitizing medication which is used to selectively destroy target tissue. The photosensitizing medication is concentrated in P. acne and sebaceous glands and upon activation of a light source such as IPL or red or blue light a localized reaction occurs resulting in destruction of P acne.
Photodynamic therapy became available in the year 2000 for the treatment of acne. Over the next decade there has been variations in the incubation time, type of activating light (wavelength nm, dosimetry J/cm2, irradiance W/cm2) rendering it difficult to compare results.
Treatments include prescription gels, cream applied to the skin and oral treatments such as antibiotics, anti-androgens and isotretinoin.
Treatment plans are devised by Dr Yip, the dermatologist and treatment is overseen by our qualified nurse.
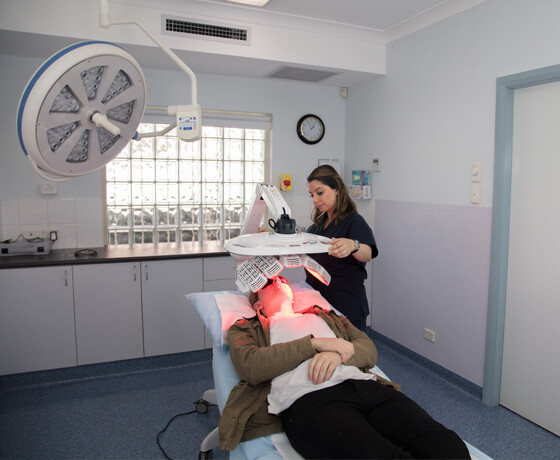
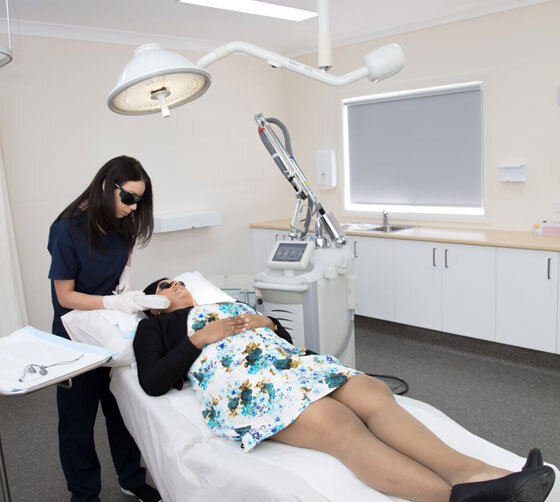
Photodynamic therapy for Acne in detail…
Firstly, a photosensitising agent most commonly a 5% solution of ALA (aminolevulinic acid) is applied to the skin under occlusive dressing for up to 3 hours. This incubation time allows the photosensitising agent to be absorbed into the skin and into the sebaceous glands. Next red or blue light is shone on the skin for 15-20minutes. This light activates the photosensitising agent which kills the acne bacteria, P. acne and helps shrink the sebaceous glands. More recently IPL, pulsed dye lasers and other lasers have been used as sources of light in PDT for acne.
The main difference between lasers and LED light devices is that lasers tend to use a smaller, more focused area of the skin and emit stronger light to the area when compared to LED devices. The advantage of using lasers is that they may require a shorter incubation time with the photosensitiser.
Increasingly dermatologists have been using IPL for PDT therapy in the management of acne. IPL uses high powered light sources that flash light onto the skin. Unlike lasers and LED light devices, which uses a specific wavelength, IPL shines broad-spectrum light that includes wavelengths of 500 to 1200nm.
The photosensitisers used are ALA (aminolevulinic acid) and MAL (methyl-aminolevulinate). MAL may be effective as a photosensitiser as it has a higher affinity for lipids such as sebaceous glands and sebum than ALA. MAL may also achieve deeper skin penetration than ALA. Incubation time is decreased with lasers and IPL devices to 45 minutes compared to LED devices.
Side effects of PDT
This include redness, swelling, itching, peeling and some crusting for a week or two as well as occasional hyperpigmentation that can last for a month after the procedure and is more common in people of darker skin types. Rarely some patients may experience a flare of acne that is transient and then spontaneously subsides. As the skin is sensitive to light it is important to stay completely out of the sun and avoid bright indoor light for 2 days after treatment.
Side effects vary with the type of photosensitiser used. MAL tends to produce more severe pain during treatment and has a higher chance of hyperpigmentation. Research is underway looking at other photosensitisers that produce less pain, greater efficacy and shorter incubation times. Indole-3- acetic acid (IAA) with green light is currently under investigation.
Long term effects
Photodynamic therapy is still a relatively new treatment in the management of acne. PDT works by shrinking oil glands. Patients with acne tend to have larger sebaceous glands that produce more oil than people without acne.
Long term results suggests an average reduction in inflammatory acne of about 60% after 3 months. The best results are seen in people with more severe forms of acne. A large systemic review article published in 2016 reviewed all available clinical studies that evaluated the use of PDT in acne. The reviewers concluded that PDT is effective, and is effective for the more severe cases of acne. It worked well on acne in various sites include the back and chest.
Long term followup of these patients is lacking. More extensive studies on a larger population with a control groups are needed to reach conclusive results on the effectiveness of PDT on acne.